Herniated Disc
A common cause of neck & back pain
What is a Spinal or Intervertebral disc?
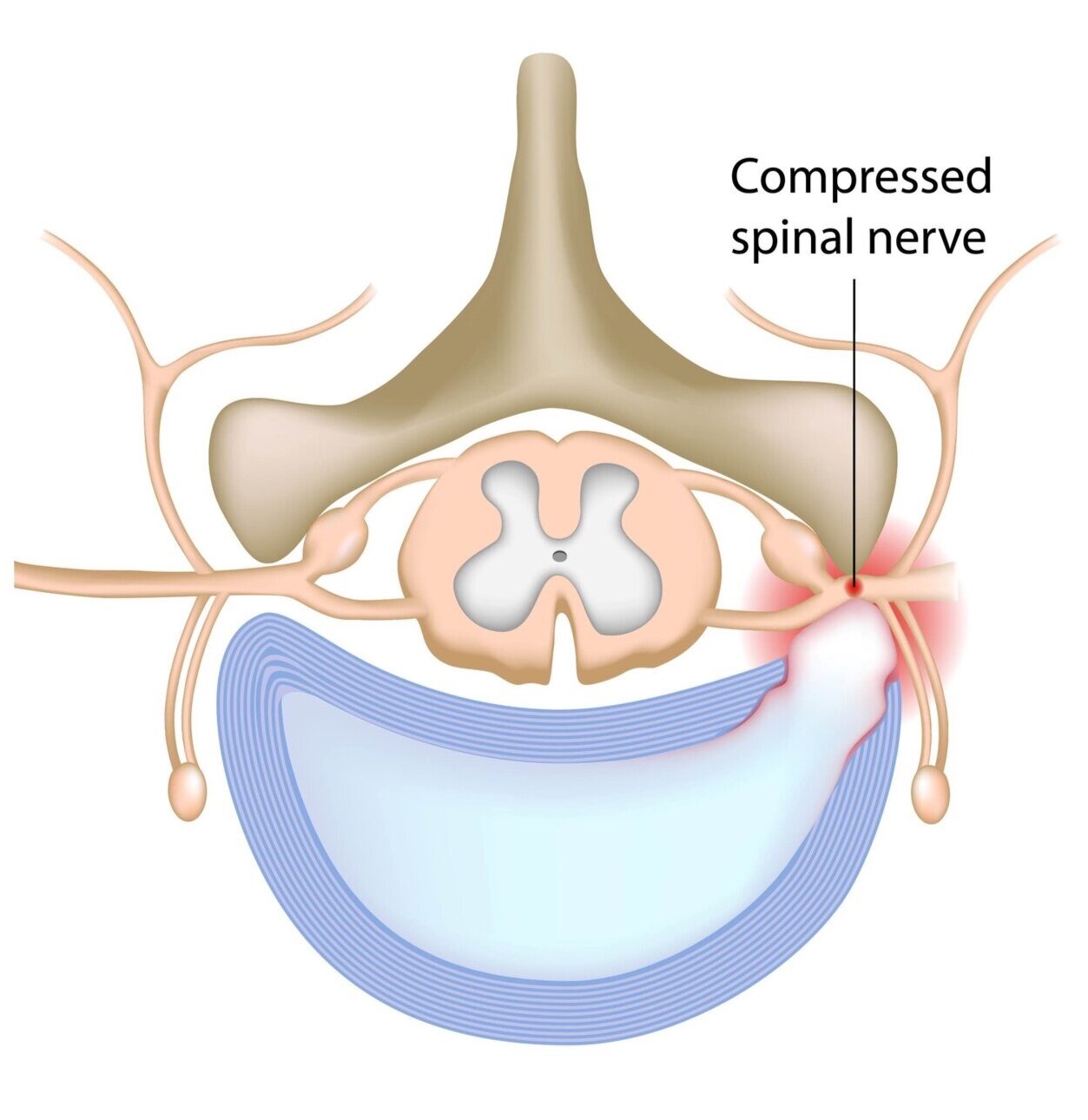
It is a rubbery cushion (disc) between individual bones of the spine (vertebrae). A spinal disc is somewhat like a jelly donut with a soft center (nucleus pulposus) within a hard exterior (annulus fibrosus).
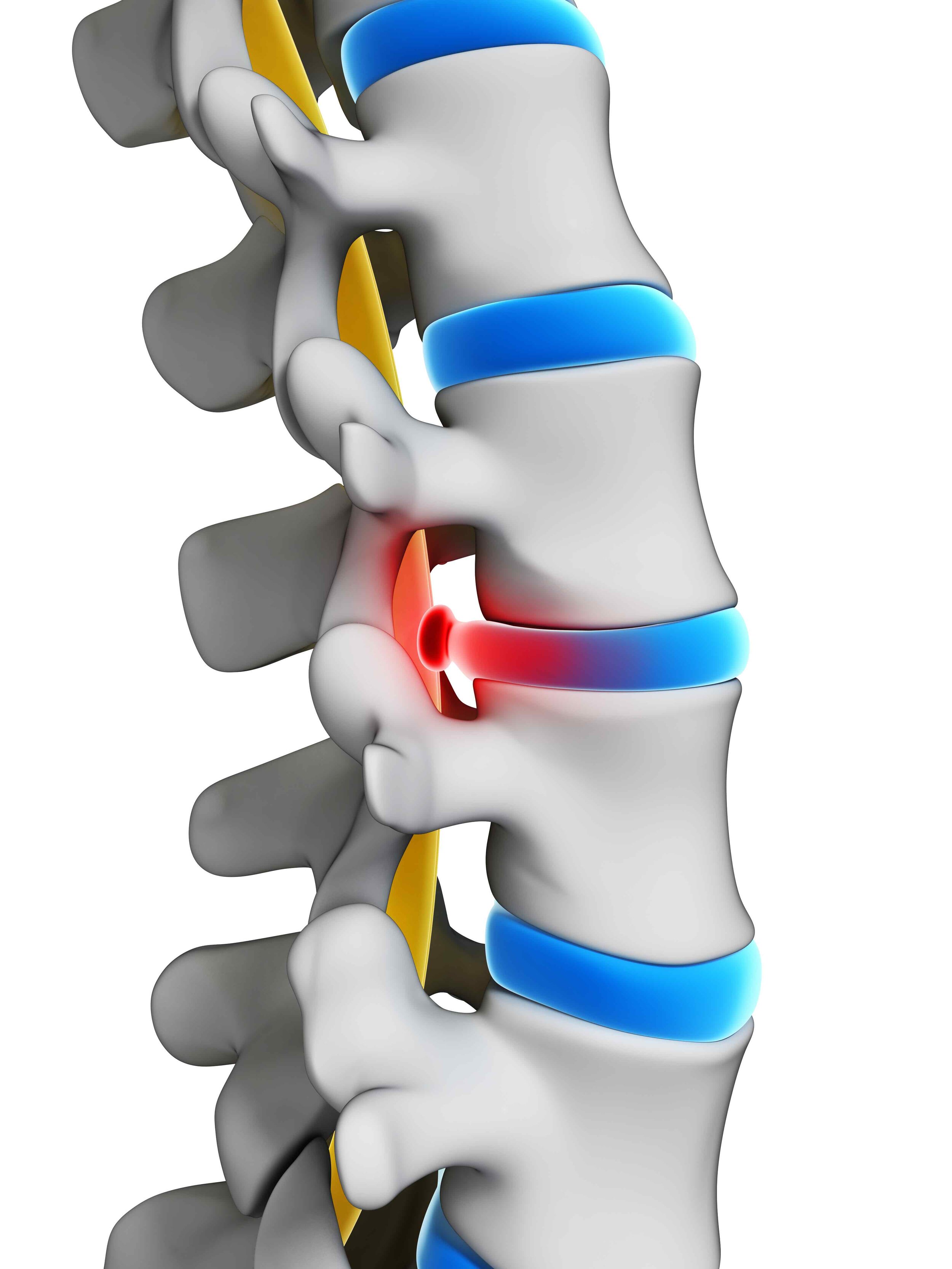
What is Spinal Disc Herniation?
Spinal disc herniation occurs when some of the softer "jelly" present in the center of the disc pushes out through a crack in the tough exterior. A herniated disc can irritate nearby nerves and result in back pain or neck pain, numbness or weakness in an arm or leg. Herniated disc is also referred to as a slipped disc or a ruptured disc.
What are the risk factors for disc herniation?
Risk factors associated with disc herniation include:
Aging
Injury
Obesity
Lifting heavy objects
“I have been going to his office for many years... I have recommended him to many family and friends and they all have had a pleasurable and rewarding outcomes with Dr. Goswami.”
— Diane Loesner
How do you diagnose disc herniation?
Medical history and physical examination can usually identify any serious conditions. A MRI may be ordered to rule out specific causes of pain.
What do you treat disc herniation?
The goal of our treatment is functional restoration. Functional restoration program seeks to return patients to levels of activity that they were able to perform prior to suffering from back pain. Usually a combination of conservative therapy, physical therapy and interventional therapy is needed.
Conservative treatment such as applying heat or ice to the painful area or taking over-the-counter pain relievers such as Tylenol or Ibuprofen.
Physical Therapy/ Muscle strengthening regimen
Certain medication such as anticonvulsants and antidepressants are known to benefit patients suffering from herniated disc disease.
Rarely minimally invasive surgery such as endoscopic discectomy might be needed
What is Epidural Steroid Injection?
During epidural steroid injection, a small amount of steroid is injected into the epidural space around the spinal cord and spinal nerves. The anti-inflammatory effects of the corticosteroid is responsible for providing pain relief.
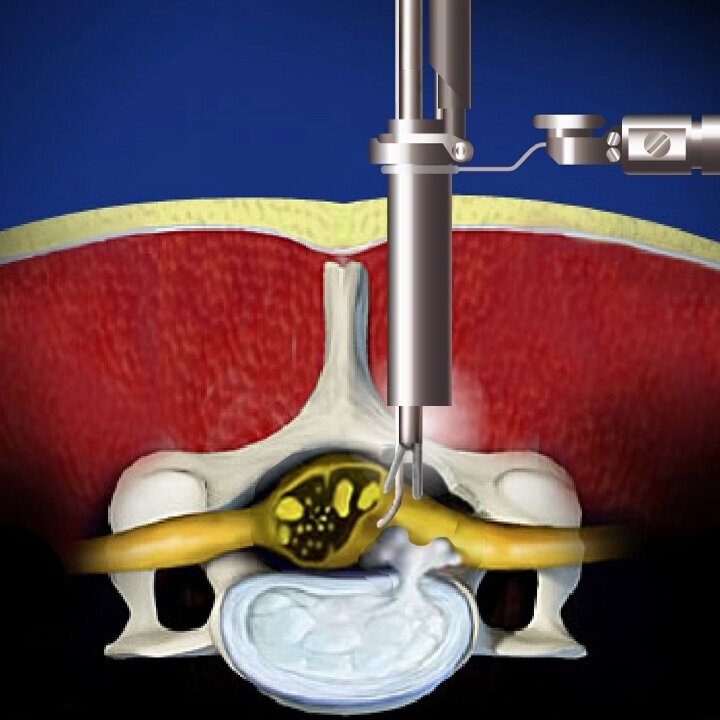
What is Endoscopic Discectomy?
A small metal tube, the size of a pencil, and a tiny camera (endoscope) is inserted into the herniated disc space. Under the guidance of real-time x-ray image and a magnified live video feed, the fragment of the herniated disc is removed.